|
Hypertriglyceridemia
may actually be an acute phase reactant in the
plasma
......................................................................................................................................................................
Mehmet Rami
Helvaci (1)
Mursel Davarci
(2)
Orhan Veli Ozkan
(3)
Ersan Semerci
(3)
Abdulrazak Abyad
(4)
Lesley Pocock
(5)
(1) Specialist of Internal
Medicine, M.D.
(2) Specialist of Urology, M.D.
(3) Specialist of General Surgery, M.D.
(4) Middle-East Academy for Medicine of Aging,
Chairman, M.D., MPH, MBA, AGSF
(5) medi+WORLD International
Correspondence:
Mehmet Rami Helvaci, M.D.
07400, ALANYA, Turkey
Phone: 00-90-506-4708759
Email: mramihelvaci@hotmail.com
|
ABSTRACT
Background: We tried to understand whether
or not there is a significant relationship
between cholelithiasis or cholecystectomy
and plasma lipids.
Methods: The study was performed in
Internal Medicine Polyclinics on routine
check up patients. All cases either with
cholelithiasis or cholecystectomy for cholelithiasis
were put into the first, and age and sex-matched
control cases were put into the second groups.
Results: One hundred and forty-four
cases either with cholelithiasis or cholecystectomy
for cholelithiasis were detected among 3,437
cases, totally (4.1%). One hundred and sixteen
(80.1%) of them were females with a mean
age of 53.6 years. Obesity (54.8% versus
43.7%, p<0.01), body mass index (BMI)
(31.0 versus 28.9 kg/m2, p<0.01), and
hypertension (26.3% versus 13.1%, p<0.001)
were significantly higher in the cholelithiasis
or cholecystectomy group. Although the prevalence
of hyperbetalipoproteinemia was significantly
lower in the cholelithiasis or cholecystectomy
group (9.7% versus 18.0%, p<0.05), hypertriglyceridemia
(25.0% versus 18.0%, p<0.05) was significantly
higher in them.
Conclusions: There are significant relationships
between cholelithiasis and parameters of
the metabolic syndrome including age, female
sex, BMI, obesity, hypertension, and hypertriglyceridemia,
so cholelithiasis may also be found among
the terminal consequences of the metabolic
syndrome. Although the significantly lower
prevalence of hyperbetalipoproteinemia is
probably due to the decreased amount of
bile acids secreted during entrance of food
into the duodenum and decreased amount of
cholesterol absorbed in patients with cholelithiasis
or cholecystectomy, the higher prevalence
of hypertriglyceridemia may actually indicate
its primary role as an acute phase reactant
in the plasma.
Key words: Hypertriglyceridemia, metabolic
syndrome, acute phase reactant, cholelithiasis,
cholecystectomy
|
Chronic endothelial damage may
be the most common kind of vasculitis and the
leading cause of aging, morbidity, and mortality
in human beings (1, 2). Much higher blood pressure
(BP) of the afferent vasculature may be the major
underlying cause by inducing recurrent injuries
on endothelium, and probably whole afferent vasculature
including capillaries are involved in the process.
Thus the term of venosclerosis is not as famous
as atherosclerosis in the literature. Secondary
to the chronic endothelial inflammation, edema,
and fibrosis, vascular walls become thickened,
their lumens are narrowed, and they lose their
elastic natures that reduce blood flow to terminal
organs and increase systolic BP further. Some
of the well-known causes and indicators of the
inflammatory process are sedentary life style,
animal-rich diet, overweight, smoking, alcohol,
hypertriglyceridemia, hyperbetalipoproteinemia,
dyslipidemia, impaired fasting glucose, impaired
glucose tolerance, white coat hypertension, and
chronic inflammatory processes including rheumatologic
disorders, chronic infections, and cancers for
the development of terminal complications including
obesity, hypertension, diabetes mellitus (DM),
cirrhosis, peripheric artery disease (PAD), chronic
obstructive pulmonary disease (COPD), chronic
renal disease (CRD), coronary artery disease (CAD),
mesenteric ischemia, osteoporosis, and stroke,
all of which terminate with early aging and premature
death. Although early withdrawal of causative
factors may prevent irreversible complications,
after development of cirrhosis, COPD, CRD, CAD,
PAD, or stroke, endothelial changes cannot be
reversed completely due to the fibrotic natures
of them. The accelerator factors and terminal
consequences were researched under the titles
of metabolic syndrome, aging syndrome, or accelerated
endothelial damage syndrome in the literature,
extensively (3-6). On the other hand, gallstones
are also found among one of the most common health
problems in developed countries (7), and they
are particularly frequent in women above the age
of 40 years (8). Most of the gallstones are found
in the gallbladder with the definition of cholelithiasis.
Its pathogenesis is uncertain and appears to be
influenced by genetic and environmental factors
(9). Excess weight is a well-known and age-independent
risk factor for cholelithiasis (10). Delayed bladder
emptying, decreased small intestinal motility,
and sensitivity to cholecystokinin were associated
with obesity and cholelithiasis (11). An increased
risk was confirmed in obese diabetics with hypertriglyceridemia
(12), and plasma cholesterol levels were also
found related with cholelithiasis (13). We tried
to understand whether or not there is a significant
relationship between cholelithiasis or cholecystectomy
and plasma lipids.
The study was performed in Internal
Medicine Polyclinics of the Dumlupinar and Mustafa
Kemal Universities on routine check up on patients
between August 2005 and November 2007. We took
consecutive patients below the age of 70 years
to avoid debility induced weight loss in elders.
Their medical histories including smoking habit,
hypertension, DM, dyslipidemia, and already used
medications and performed operations were learnt,
and a routine check up procedure including fasting
plasma glucose (FPG), triglyceride, high density
lipoprotein cholesterol (HDL-C), low density lipoprotein
cholesterol (LDL-C), and an abdominal ultrasonography
was performed. Patients with devastating illnesses
including type 1 DM, malignancies, acute or chronic
renal failure, chronic liver diseases, hyper-
or hypothyroidism, and heart failure were excluded
to avoid their possible effects on weight. Current
daily smokers at least for the last six months
and cases with a history of five pack-years were
accepted as smokers. Cigar or pipe smokers were
excluded. Body mass index (BMI) of each case was
calculated by the measurements of the Same Physician
instead of verbal expressions since there is evidence
that heavier individuals systematically underreport
their weight (14). Weight in kilograms is divided
by height in meters squared, and underweight is
defined as a BMI value of lower than 18.5, normal
weight as lower than 24.9, overweight as lower
than 29.9, and obesity as 30.0 kg/m2 or greater
(15). Cases with an overnight FPG level of 126
mg/dL or greater on two occasions or already receiving
antidiabetic medications were defined as diabetics
(15). An oral glucose tolerance test with 75-gram
glucose was performed in cases with a FPG level
between 110 and 125 mg/dL, and diagnosis of cases
with a 2-hour plasma glucose level 200 mg/dL or
higher is DM (15). Patients with dyslipidemia
were detected, and we used the National Cholesterol
Education Program Expert Panel's recommendations
for defining dyslipidemic subgroups (15). Dyslipidemia
is diagnosed when LDL-C is 160 or higher and/or
triglyceride is 200 or higher and/or HDL-C is
lower than 40 mg/dL. Office BP was checked after
a 5-minute of rest in seated position with a mercury
sphygmomanometer on three visits, and no smoking
was permitted during the previous 2 hours. A 10-day
twice daily measurement of blood pressure at home
(HBP) was obtained in all cases, even in normotensives
in the office due to the risk of masked hypertension
after a 10-minute education about proper BP measurement
techniques (16). The education included recommendation
of upper arm while discouraging wrist and finger
devices, using a standard adult cuff with bladder
sizes of 12 x 26 cm for arm circumferences up
to 33 cm in length and a large adult cuff with
bladder sizes of 12 x 40 cm for arm circumferences
up to 50 cm in length, and taking a rest at least
for a period of 5 minutes in the seated position
before measurement. An additional 24-hour ambulatory
BP monitoring was not required due to the equal
efficacy of the method with HBP measurement to
diagnose hypertension (17). Eventually, hypertension
is defined as a BP of 135/85 mmHg or greater on
HBP measurements (16). Cholelithiasis was diagnosed
ultrasonographically. Eventually, all cases either
with presenting cholelithiasis or cholecystectomy
for cholelithiasis were put into the first and
age and sex-matched control cases were put into
the second groups. The mean BMI values and prevalences
of smoking, normal weight, overweight, obesity,
hypertension, DM, hypertriglyceridemia, hyperbetalipoproteinemia,
and dyslipidemia were compared between the two
groups. Mann-Whitney U test, Independent-Samples
t test, and comparison of proportions were used
as the methods of statistical analyses.
Although the exclusion criteria,
25 cases with already presenting asymptomatic
cholelithiasis and 119 cases with cholecystectomy
for cholelithiasis were detected among 3.437 cases,
totally (4.1%). One hundred and sixteen (80.1%)
of them were females with a mean age of 53.6 years,
so cholelithiasis is mainly a disorder of females
in their fifties. Prevalences of smoking were
similar in the cholelithiasis and control groups
(18.0% versus 19.4%, p>0.05, respectively).
Interestingly, 92.3% (133 cases) of the cholelithiasis
group had excess weight and only 7.6% (11 cases)
of them had normal weight. There was not any patient
with underweight among the study cases. Obesity
was significantly higher (54.8% versus 43.7%,
p<0.01) and normal weight was significantly
lower (7.6% versus 18.0%, p<0.01) in the cholelithiasis
group. Mean BMI values were 31.0 and 28.9 kg/m2,
(p<0.01) in the two groups. Probably parallel
to the higher mean BMI values, prevalence of hypertension
(26.3% versus 13.1%, p<0.001) was also higher
in the cholelithiasis group, significantly. Although
the prevalences of DM (20.8% versus 19.4%, p>0.05)
and dyslipidemia (31.9% versus 29.8%, p>0.05)
were also higher in the cholelithiasis groups,
differences were nonsignificant probably due to
the small sample sizes of the groups. Although
the prevalence of hyperbetalipoproteinemia was
significantly lower in the cholelithiasis or cholecystectomy
group (9.7% versus 18.0%, p<0.05), hypertriglyceridemia
(25.0% versus 18.0%, p<0.05) was significantly
higher in them (Table 1).
Table 1: Comparison of
cases with and without cholelithiasis
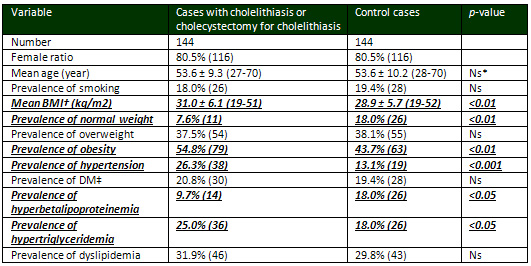
*Nonsignificant (p>0.05)
†Body mass index ‡Diabetes mellitus
Bile is formed in the liver as
an isosmotic solution of bile acids, cholesterol,
phospholipids, bilirubin, and electrolytes. The
liver synthesizes water-soluble bile acids from
water-insoluble cholesterol. About 50% of bile
secreted during the fasting state passes into
the gallbladder via the cystic duct. So gallbladder
filling is facilitated during fasting. Up to 90%
of water in the gallbladder bile is absorbed as
an electrolyte solution, so bile acids are concentrated
in the gallbladder and little amount of bile flows
from the liver during fasting. Food entering the
duodenum stimulates gallbladder contraction, releasing
much of the body pool of bile acids to mix with
food content and perform its several functions
including solubilization of dietary cholesterol,
fats, and fat-soluble vitamins to facilitate their
absorption in the form of mixed micelles, causing
water secretion by the colon promoting catharsis,
excretion of bilirubin as degradation products
of heme compounds from worn-out red blood cells,
excretion of drugs and ions from the body, and
secretion of various proteins important for the
gastrointestinal functions. About 90% of bile
acids is reabsorbed by the terminal ileum into
the portal system. Bile salts
are efficiently extracted by the liver, and secreted
back into bile, so bile acids undergo enterohepatic
circulation 10 to 12 times per day. The most clinical
disorders of the extrahepatic biliary tract are
related with the gallstones. In the USA, 20% of
people above the age of 65 years have gallstones,
and each year more than 500,000 patients undergo
cholecystectomy. Factors increasing the probability
of gallstones include age, female sex, and obesity.
Highly water-insoluble cholesterol is the major
component of most gallstones. Biliary cholesterol
is solubilized in the bile salt-phospholipid micelles
and phospholipid vesicles. The amount of cholesterol
carried in micelles and vesicles varies with the
bile salt secretion rate. In another perspective,
cholelithiasis may actually be a natural defence
mechanism of the body to decrease amount of bile
acids secreted during entrance of food into the
duodenum and decrease amount of cholesterol absorbed.
Similarly, bile acid sequestrants including cholestyramine
and cholestipol effectively lower serum LDL-C
by binding bile acids in intestine and interrupting
enterohepatic circulation of them.
Excess weight leads to both structural
and functional abnormalities of many systems of
the body. Recent studies revealed that adipose
tissue produces leptin, tumor necrosis factor-alpha,
plasminogen activator inhibitor-1, adiponectin,
and other cytokines which act as acute phase reactants
in the plasma (18, 19). For example, the cardiovascular
field has recently shown a great interest in the
role of inflammation in the development of atherosclerosis
and numerous studies indicated that inflammation
plays a significant role in the pathogenesis of
atherosclerosis and thrombosis (1, 2). On the
other hand, individuals with excess weight have
an increased blood volume as well as an increased
cardiac output thought to be the result of increased
oxygen demand of the excessive fat tissue. The
prolonged increase in blood volume can lead to
myocardial hypertrophy and decreased compliance
in addition to the common comorbidity of hypertension.
In addition to them, the prevalences of high FPG,
high serum total cholesterol, and low HDL-C increased
parallel to the higher BMI values (20). Combination
of these cardiovascular risk factors will eventually
lead to an increase in left ventricular stroke
with higher risks of arrhythmias, cardiac failure,
and sudden cardiac death. Similarly, the prevalences
of CAD and stroke increased parallel with the
higher BMI values in some other studies (20, 21),
and risk of death from all causes including cancers
increased throughout the range of moderate to
severe weight excess in all age groups (22). As
another consequence of excess weight on health,
cholelithiasis cases had a significantly higher
BMI value in the present study (31.0 versus 28.9
kg/m2, p<0.01) similar to some other reports
(8, 9). Probably as a consequence of the higher
BMI values, the prevalences of hypertension (26.3%
versus 13.1%, p<0.001) and hypertriglyceridemia
(25.0% versus 18.0%, p<0.05) were also higher
in the cholelithiasis group. The relationships
between excess weight and elevated BP and hypertriglyceridemia
were described in the metabolic syndrome (23),
and clinical manifestations of the syndrome included
obesity, dyslipidemia, hypertension, insulin resistance,
and proinflammatory and prothrombotic states (24).
The increased risk of cholelithiasis in obese
diabetics with hypertriglyceridemia may also be
an indicator of its association with the metabolic
syndrome (10, 23). Similarly, prevalences of smoking
(42.2% versus 28.4%, p<0.01), excess weight
(83.6% versus 70.6%, p<0.01), DM (16.3% versus
10.3%, p<0.05), and hypertension (23.2% versus
11.2%, p<0.001) were all higher in the hypertriglyceridemia
cases in another study (25). It is a well-known
fact that smoking causes a chronic inflammatory
process in the respiratory tract, lungs, and vascular
endothelium all over the body terminating with
an accelerated atherosclerosis, end-organ insufficiencies,
early aging, and premature death thus it should
be included among the major parameters of the
metabolic syndrome. On the other hand, smoking-induced
weight loss is probably related with the smoking-induced
endothelial inflammation all over the body since
loss of appetite is one of the main symptoms of
disseminated inflammation in the body. In another
explanation, smoking-induced loss of appetite
is an indicator of being ill instead of being
healthy during smoking (26-28). Buerger's disease
(thromboangiitis obliterans) alone is also a clear
evidence to show the strong atherosclerotic effects
of smoking since this disease has not been shown
in the absence of smoking up to now. On the other
hand, as a parallel finding to the present study,
the prevalences of hyperbetalipoproteinemia were
similar in the hypertriglyceridemia and control
groups (18.9% versus 16.3%, p>0.05, respectively)
in the above study (25).
Although the mean age, female
sex, BMI, obesity, hypertension, and hypertriglyceridemia
indicated significant differences in the cholelithiasis
or cholecystectomy group in the present study,
there was no significant difference for the lipid
parameters in another study (29). Whereas total
cholesterol, triglycerides, and LDL-C were significantly
reduced in patients on day 3 of surgery and 6
months after the cholecystectomy in another one
(30). Similar to our results, significantly higher
prevalence of cholelithiasis was found in patients
with nonalcoholic fatty liver disease (NAFLD)
(47% versus 26%, p<0.0001), and type 2 DM,
overweight, obesity, and cholelithiasis were identified
as independent predictors of NAFLD (31). Fifty
six percent of patients with cholelithiasis had
NAFLD compared with 33% of patients without (p<0.0001)
(31). Age above 50 years, triglycerides above
1.7 mmol/l, overweight, obesity, and total cholesterol
concentration were the independent predictors
of cholelithiasis (31). So NAFLD may represent
a pathogenetic link between the metabolic syndrome
and cholelithiasis (31). Similarly, patients with
type 2 DM had higher probability of having cholelithiasis,
and age, female sex, and BMI were independently
associated with cholelithiasis (32). Obesity may
lead to fatty infiltration causing organ dysfunctions,
and the higher BMI values were associated with
steatocholecystitis in another study (33). As
an opposite finding to our results, serum LDL-C
values of patients with cholelithiasis above the
age of 40 years were significantly elevated (p<0.05)
in another one (34).
Although ATP II determined
the normal triglyceride value as lower than 200
mg/dL (35), WHO in 1999 (36) and ATP III in 2001
(13) reduced this normal limit as lower than 150
mg/dL. Although these cutpoints are usually used
to define limits of the metabolic syndrome, whether
or not more lower limits provide additional benefits
for human beings is unclear. In a previous study,
patients with a triglyceride value lower than
60 mg/dL were collected into the first, lower
than 100 mg/dL into the second, lower than 150
mg/dL into the third, lower than 200 mg/dL into
the fourth, and equal to or greater than 200 mg/dL
were collected into the fifth groups, respectively
(23). Prevalence of smoking was the highest in
the fifth group which may also indicate inflammatory
roles of smoking and hypertriglyceridemia in the
metabolic syndrome. The mean body weight increased
continuously, parallel to the increasing value
of triglyceride. As the most surprising result,
the prevalences of hypertension, type 2 DM, and
CAD, as some of the terminal end points of the
metabolic syndrome, showed their most significant
increases after the triglyceride value of 100
mg/dL (23). As one of our opinion, significantly
increased mean age by the increased triglyceride
values may be secondary to aging induced decreased
physical and mental stresses, which eventually
terminates with onset of excess weight and other
parameters and terminal end points of the metabolic
syndrome. Interestingly, the mean age increased
from the lowest triglyceride having group towards
the triglyceride value of 200 mg/dL, then decreased.
The similar trend was also seen in the mean LDL-C
and BMI values, and prevalence of WCH. These trends
may be due to the fact that although the borderline
high triglyceride values (150-199 mg/dL) is seen
together with overweight, obesity, physical inactivity,
smoking, and alcohol like acquired causes, the
high triglyceride (200-499 mg/dL) and very high
triglyceride values (500 mg/dL and higher) are
usually secondary to both acquired and secondary
causes such as type 2 DM, chronic renal failure,
and genetic patterns (13). But although the underlying
causes of the high and very high triglyceride
values may be a little bit different, probably
risks of the terminal end points of the metabolic
syndrome do not change in these groups, too. For
example, prevalences of hypertension and type
2 DM were the highest in the highest triglyceride
value having group in the above study (23). Eventually,
although some authors reported that lipid assessment
in vascular disease can be simplified by measurement
of either total and HDL-C levels without the need
of triglyceride (37), the present study and most
others indicated a causal association between
triglyceride-mediated pathways and parameters
of the metabolic syndrome (38). Similarly, another
study indicated moderate and highly significant
associations between triglyceride values and CAD
in Western populations (39).
As a conclusion, there are significant relationships
between cholelithiasis and parameters of the metabolic
syndrome including age, female sex, BMI, obesity,
hypertension, and hypertriglyceridemia, so cholelithiasis
may also be found among the terminal consequences
of the metabolic syndrome. Although the significantly
lower prevalence of hyperbetalipoproteinemia is
probably due to the decreased amount of bile acids
secreted during entrance of food into the duodenum
and decreased amount of cholesterol absorbed in
patients with cholelithiasis or cholecystectomy,
the higher prevalence of hypertriglyceridemia
may actually indicate its primary role as an acute
phase reactant in the plasma.
1. Widlansky ME, Gokce N, Keaney JF Jr, Vita JA.
The clinical implications of endothelial dysfunction.
J Am Coll Cardiol 2003; 42: 1149-1160.
2. Ridker PM. High-sensitivity C-reactive protein:
Potential adjunct for global risk assessment in
the primary prevention of cardiovascular disease.
Circulation 2001; 103: 1813-1818.
3. Eckel RH, Grundy SM, Zimmet PZ. The metabolic
syndrome. Lancet 2005; 365: 1415-1428.
4. Helvaci MR, Kaya H, Sevinc A, Camci C. Body
weight and white coat hypertension. Pak J Med
Sci 2009; 25: 6: 916-921.
5. Helvaci MR, Aydin LY, Aydin Y. Digital clubbing
may be an indicator of systemic atherosclerosis
even at microvascular level. HealthMED 2012; 6:
3977-3981.
6. Helvaci MR, Aydin Y, Gundogdu M. Atherosclerotic
effects of smoking and excess weight. J Obes Wt
Loss Ther 2012; 2: 7.
7. Tazuma S. Gallstone disease: Epidemiology,
pathogenesis, and classification of biliary stones
(common bile duct and intrahepatic). Best Pract
Res Clin Gastroenterol 2006; 20: 1075-1083.
8. Katsika D, Grjibovski A, Einarsson C, Lammert
F, Lichtenstein P, Marschall HU. Genetic and environmental
influences on symptomatic gallstone disease: a
Swedish study of 43,141 twin pairs. Hepatology
2005; 41: 1138-1143.
9. Lammert F, Sauerbruch T. Mechanisms of disease:
the genetic epidemiology of gallbladder stones.
Nat Clin Pract Gastroenterol Hepatol 2005; 2:
423-433.
10. Erlinger S. Gallstones in obesity and weight
loss. Eur J Gastroenterol Hepatol 2000; 12: 1347-1352.
11. Mathus-Vliegen EM, Van Ierland-Van Leeuwen
ML, Terpstra A. Determinants of gallbladder kinetics
in obesity. Dig Dis Sci 2004; 49: 9-16.
12. Fraquelli M, Pagliarulo M, Colucci A, Paggi
S, Conte D. Gallbladder motility in obesity, diabetes
mellitus and coeliac disease. Dig Liver Dis 2003;
35: 12-16.
13. Devesa F, Ferrando J, Caldentey M, Borghol
A, Moreno MJ, Nolasco A, et al. Cholelithiasic
disease and associated factors in a Spanish population.
Dig Dis Sci 2001; 46: 1424-1436.
14. Bowman RL, DeLucia JL. Accuracy of selfreported
weight: a meta-analysis. Behav Ther 1992; 23:
637-635.
15. Third Report of the National Cholesterol Education
Program (NCEP) Expert Panel on Detection, Evaluation,
and Treatment of High Blood Cholesterol in Adults
(Adult Treatment Panel III) final report. Circulation
2002; 106: 3143-3421.
16. O'Brien E, Asmar R, Beilin L, Imai Y, Mallion
JM, Mancia G, et al. European Society of Hypertension
recommendations for conventional, ambulatory and
home blood pressure measurement. J Hypertens 2003;
21: 821-848.
17. Helvaci MR, Seyhanli M. What a high prevalence
of white coat hypertension in society! Intern
Med 2006; 45: 671-674.
18. Funahashi T, Nakamura T, Shimomura I, Maeda
K, Kuriyama H, Takahashi M, et al. Role of adipocytokines
on the pathogenesis of atherosclerosis in visceral
obesity. Intern Med 1999; 38: 202-206.
19. Yudkin JS, Stehouwer CD, Emeis JJ, Coppack
SW. C-reactive protein in healthy subjects: associations
with obesity, insulin resistance, and endothelial
dysfunction: a potential role for cytokines originating
from adipose tissue? Arterioscler Thromb Vasc
Biol 1999; 19: 972-978.
20. Zhou B, Wu Y, Yang J, Li Y, Zhang H, Zhao
L. Overweight is an independent risk factor for
cardiovascular disease in Chinese populations.
Obes Rev 2002; 3: 147-156.
21. Zhou BF. Effect of body mass index on all-cause
mortality and incidence of cardiovascular diseases
- report for meta-analysis of prospective studies
open optimal cut-off points of body mass index
in Chinese adults. Biomed Environ Sci 2002; 15:
245-252.
22. Calle EE, Thun MJ, Petrelli JM, Rodriguez
C, Heath CW Jr. Body-mass index and mortality
in a prospective cohort of U.S. adults. N Engl
J Med 1999; 341: 1097-1105.
23. Helvaci MR, Kaya H, Gundogdu M. Association
of increased triglyceride levels in metabolic
syndrome with coronary artery disease. Pak J Med
Sci 2010; 26: 667-672.
24. Tonkin AM. The metabolic syndrome(s)? Curr
Atheroscler Rep 2004; 6: 165-166.
25. Helvaci MR, Aydin LY, Maden E, Aydin Y. What
is the relationship between hypertriglyceridemia
and smoking? Middle East J Age and Ageing 2011;
8: 6.
26. Hughes JR, Hatsukami DK. Effects of three
doses of transdermal nicotine on post-cessation
eating, hunger and weight. J Subst Abuse 1997;
9: 151-159.
27. Miyata G, Meguid MM, Varma M, Fetissov SO,
Kim HJ. Nicotine alters the usual reciprocity
between meal size and meal number in female rat.
Physiol Behav 2001; 74: 169-176.
28. Laaksonen M, Rahkonen O, Prattala R. Smoking
status and relative weight by educational level
in Finland, 1978-1995. Prev Med 1998; 27: 431-437.
29. Cojocaru C, Pandele GI. Metabolic profile
of patients with cholesterol gallstone disease.
Rev Med Chir Soc Med Nat Iasi 2010;114: 677-682.
30. Malik AA, Wani ML, Tak SI, Irshad I, Ul-Hassan
N. Association of dyslipidaemia with cholilithiasis
and effect of cholecystectomy on the same. Int
J Surg 2011; 9: 641-642.
31. Koller T, Kollerova J, Hlavaty T, Huorka M,
Payer J. Cholelithiasis and markers of nonalcoholic
fatty liver disease in patients with metabolic
risk factors. Scand J Gastroenterol 2012; 47:
197-203.
32. Sodhi JS, Zargar SA, Khateeb S, Showkat A,
Javid G, Laway BA, et al. Prevalence of gallstone
disease in patients with type 2 diabetes and the
risk factors in North Indian population: a case
control study. Indian J Gastroenterol 2014; 33:
507-511.
33. Yoon JH, Kim YJ, Baik GH, Kim YS, Suk KT,
Kim JB, et al. The Impact of Body Mass Index as
a Predictive Factor of Steatocholecystitis. Hepatogastroenterology
2014; 61: 902-907.
34. Batajoo H, Hazra NK. Analysis of serum lipid
profile in cholelithiasis patients. J Nepal Health
Res Counc 2013; 11: 53-55.
35. National Cholesterol Education Program. Second
report of the expert panel on detection, evaluation,
and treatment of high blood cholesterol in adults
(Adult Treatment Panel II). Circulation 1994;
89: 1333-1445.
36. World Health Organization. Definition, diagnosis
and classification of diabetes mellitus and its
complications. Report of a WHO consultation 1999.
37. Di Angelantonia E, Sarwar N, Perry P, Kaptoge
S, Ray KK, Thompson A, et al. Major lipids, apolipoproteins,
and risk of vascular disease. JAMA 2009; 302:
1993-2000.
38. Sarwar N, Sandhu MS, Ricketts SL, Butterworth
AS, Di Angelantonia E, Boekholdt SM, et al. Triglyceride-mediated
pathways and coronary disease: collaborative analysis
of 101 studies. Lancet 2010; 375: 1634-1639.
39. Sarwar N, Danesh J, Eiriksdottir G, Sigurdsson
G, Wareham N, Bingham S, et al. Triglycerides
and the risk of coronary heart disease: 10,158
incident cases among 262,525 participants in 29
Western prospective studies. Circulation 2007;
115: 450-458.
|
